According to international statistics, colorectal cancer (CRC) is the third most commonly diagnosed cancer in males and second in females.1 However in India lies, the incidence is lower as compared in Europe and North America. According to ICMR consensus document on management of CRC (2014), colon cancer ranks as 8th and rectal cancer as 9th among men and amongst women colon cancer ranks 9th while cancer rectum does not figure in top 10 cancers.
First presentation of CRC as emergency – obstruction, perforation or bleeding is not uncommon. Malignant large bowel obstruction is reported in 8-13% patients with CRC In Western studies.2,3 Another multicentre study from UK involving 286591 patients over a 15 year period (1997 – 2012) reported that 24.3% (69718 patients) needed emergency for CRC and all cause 30 and 90 day mortality was significantly higher in patients undergoing emergency surgery as compared to elective surgery.4
Management of such patients is particularly challenging as they are often elderly with significant comorbidity and histopathologic diagnosis may not be unavailable. At surgery large bowel may be hugely distended and complex resections may be required.
In the following sections, we briefly discuss the management CRC presenting as emergency through a representative case series of patients wherein the first presentation was obstruction or perforation.
Case study 1
An elderly woman in her 5th decade presented with acute intestinal obstruction. Her contrast enhanced abdominal computed tomography (CT) scan showed mass lesion in cecum – ascending colon (Figure 1).
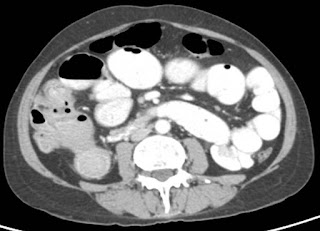
Figure 1. Carcinoma right colon with acute_Intestinal obstruction
She underwent right hemicolectomy with primary anastomosis and had an uneventful recovery. The biopsy was suggestive of adenocarcinoma T3N1. She was stared on adjuvant chemotherapy after 3 weeks and is currently well 4 years after surgery.
Case study 2
An elderly woman in her 8th decade presented with 6 months history of weight loss and progressive constipation that for last 4 days had progressed to obstipation. There was no major comorbid illness and prior to obstipation she was managing her daily activities. Her abdominal CT scan revealed obstructing lesion in rectosigmoid region with closed loop obstruction. There were multiple colorectal liver metastases in segment 2 & 3 (Figure 2 & 3).
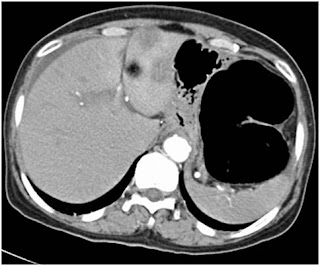
Figure 2. Abdominal CT scan with distended left colon and CLM
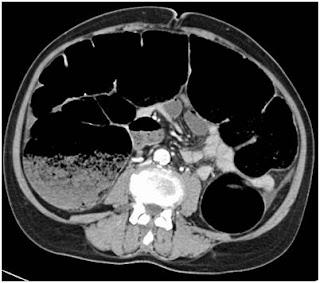
Figure 3. Abdominal CT scan showing closed obstruction of large bowel
At surgery, the whole of whole of large bowel was massively distended but the cecum was viable. Anterior resection with ascending colostomy was done. She opted for colostomy closure 8 weeks later but declined further chemotherapy. Following this second surgery she was restored to good quality of life and passed away 16 months later.
Case study 3
An elderly male with history of weight loss and progressive constipation presented to emergency room. He was a known diabetic and had undergone coronary bypass 1 year ago had low ejection fraction (35%). Abdominal CT scan is provided in Figure 4. The total white blood cell count was 39,000 mm3
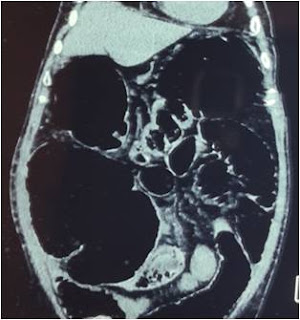
Figure 4. Closed loop obstruction of large bowel with hugely distended cecum
At surgery, there was an obstructing mass lesion in sigmoid colon with infiltration of dome of urinary bladder. The cecum appeared gangrenous. A subtotal colectomy with partial cystectomy was performed. Reconstruction was by an ileorectal anastomosis with diverting loop ileostomy. He had an uneventful postoperative recovery and was discharged on 8th postoperative day. The biopsy reported adenocarcinoma sigmoid colon T4N1 with all clear surgical margins. The ileostomy was successfully reversed 8 weeks later.
Discussion
A US study (1991 – 2005) involving 1004 patients ≥65 years with stage IV colon cancer reported that obstruction occurred a median of 7.4 months after colon cancer diagnosis and median survival after obstruction was approximately 2.5 months.5 Risk factors for presentation with obstruction included proximal location, high grade tumor, mucinous histological type and nodal stage N2.3 Another study from Australia has reported that emergency patients had 5 year survival rate of 39. 2% compared to 64.7% for elective patients (p< 0.0001) and they also had significantly more advanced Dukes C & D tumors. Also both emergency Dukes B and C groups had significantly more T4 cases.6
The current treatment options for MLBO include:
- Endoscopic stenting with self expanding metallic stent (SEMS) placement
Endoscopic stenting with SEMS can be used as a palliative therapy in patients with unresectable primary or metastatic disease. For patients with malignant large bowel obstruction where a curative surgery is deemed feasible SEMS is used as a bridge to definitive surgery thereby avoiding risks of emergency surgery, higher chances of primary anastomosis and avoiding permanent stomas in 30-40% patients.7.8 However SEMS placement may result in perforation rates ranging between 6.9 – 7.7%.8,9
- Surgery: This may be done as one, two or 3 stage procedure:
– Single stage procedure: Oncologic resection + primary anastomosis.
This is generally acceptable for obstructing carcinoma on the right side and in select patients on left side in the form of subtotal colectomy with ileorectal anastomosis.
– Two stage – (i) Oncologic resection with anastomosis + proximal diverting stoma (ii) stoma closure
– Three stage – (i) Proximal diverting stoma (ii) oncologic resection of the tumor(iii) stoma closure
The choice of treatment depends on the usual combination of patient factors (e.g. age, comorbidity, hemodynamic stability, patient preference etc), tumor factors (stage, location, degree of obstruction – partial or complete, condition of the proximal bowel e.g. bowel dilatation, viability of cecum) and available local expertise.
Hence for optimal immediate and oncological outcomes such patients should always be managed by surgical teams experienced in GI oncosurgery as well as emergency GI surgery.
References
- Torre LA1, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A. Global cancer statistics 2012. CA Cancer J Clin. 2015 Mar;65(2):87-108
- Jeanin E. van Hooft, Joyce V. Veld, 2, Dirk Arnold et al. Self-expandable metal stents for obstructing colonic and extracolonic cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline – Update 2020. Endoscopy
- Winner M, Mooney SJ, Hershman DL et al. Incidence and predictors of bowel obstruction in elderly patients with stage IV colon cancer. JAMA Surg 2013;148(8):715-22
- Askari A, Nachiappan S, Currie A et al. Who requires emergency surgery for colorectal cancer and can national screening programs reduce this need. Int J Surg 2017;42:60-68
- Winner M, Mooney SJ, Hershman DL et al. Management and outcome of bowel obstruction in patients with stage IV colon cancer. Dis Colon Rectum. 2013 Jul; 56(7): 834–843.
- Wong SK1, Jalaludin BB, Morgan MJ. Tumor pathology and long term survival in emergency colorerectal cancer. Dis Colon Rectum. 2008 Feb;51(2):223-30
- Hsu J, Sevak S. Malignant large bowel obstruction. Dis Colon Rectum 2019; 62: 1028–1032
- Amelung FJ, Borstlap WAA, Consten ECJ et al. Propensity score-matched analysis of oncological outcome between stent as bridge to surgery and emergency resection in patients with malignant left-sided colonic obstruction. Br J Surg 2019;106:1075-1086
- Tan CJ, Dasari BV, Gardiner K Systematic review and meta-analysis of randomized clinical trials of self-expanding metallic stents as a bridge to surgery versus emergency surgery for malignant left-sided large bowel obstruction. Br J Surg 2012;99:469-76
Authors:
Dr Nitin Vashistha, MS, FIAGES, FACS
Dr Dinesh Singhal, MS, FACS, DNB (Surg Gastro)
Department of Surgical Gastroenterology,
Max Super Speciality Hospital, Saket, New Delhi, India
E mail: gi.cancer.india@gmail.com

