Quiz
A 67 year non alcoholic, non smoker lady presented with dull ache in the right upper quadrant of abdomen and a progressive abdominal mass of 10 years duration. She denied any history of vomiting, weight loss or any major comorbidity. There was no icterus or peripheral lymphadenopathy. Abdominal examination revealed a large firm mass with bosselated surface in right hypochondrium extending into the right lumbar region. whipple surgery
The initial investigations were within normal range except for deranged liver functions (total bilirubin 1.5 mg/dL, aspartate transaminase 75 U/L, alanine transaminase 87 U/L, alkaline phosphatase 367 U/L, serum albumin 4 gm/L). Contrast enhanced magnetic resonance imaging (Figure A) showed a large periampullary tumor which was suggestive of nonfunctioning islet /neuroendocrine tumor or duodenal gastrointestinal stromal tumor.
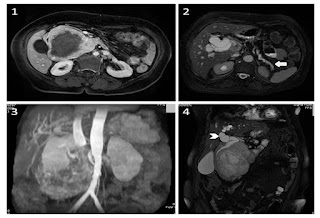
Figure A. Large periampullary tumor with central necrosis and peripheral enhancement (Image 1). Atrophic pancreas (arrow – Image 2). Compression of inferior vena cava (Image 3).Common duct with proximal biliary dilatation (arrow head – Image 4).
The patient underwent standard pancreatoduodenectomy (PD) with an uneventful recovery. The histopathology was suggestive of spindle cell tumor arising from the duodenal wall (CD 117 positive; mitotic activity < 2 / 50 high power field).
Three months after surgery she developed low appetite, loss of weight, pedal edema and abdominal distension. On investigations by the primary physician there was ascites for which ‘no cause was detected’. Six months after PD, the patient was readmitted with icterus, progressive pedal edema and ascites. Her initial work up investigations:
– Total bilirubin 4.9mg/dL, liver enzymes – within normal limits, serum proteins 5.8 gm/L;
serum albumin 1.6 gm/L
– Serum lipid profile (mg/dL): triglycerides 150; cholesterol 70; HDL 14; LDL 26; VLDL 30,
– Urine proteins nil.
– Ascitic fluid: Clear, straw colored; cell count- 50/mm3 (all lymphocytes); Proteins 1.1g/dL Albumin 0.3 g/dL, Sugar 105mg/dL; Amylase 37 IU/L; Triglycerides 30 mg/dL
Subsequently, contrast enhanced abdominal computed tomography (CECT) scan was done (Figure B).
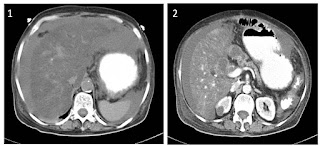
Figure B. Abdominal contrast enhanced computed tomography scan (image 1 & 2)
What is the diagnosis?
- Peritoneal carcinomatosis
- Portal vein thrombosis
- Chylous ascites
- Post PD non alcoholic steatohepatitis (NASH)
Answer
- Post PD non alcoholic steatohepatitis
This seemingly complex clinical problem has a simple solution- estimation of serum albumin – ascites gradient (SAAG) and close look at abdominal CECT (Figure B). On readmission our patient had high SAAG ascites. This ruled out options 1 & 3 – peritoneal carcinomatosis (PC) and chylous ascites (CA). There are other features against these two diagnoses as well. A potentially serious complication of PD, CA is milky fluid with triglyceride content of ≥ 110 mg / dL from drain/ drain site/ wound after 3rd postoperative day.1 In our patient, onset of ascites was delayed, it was straw colored & with triglyceride content of 30 mg/dL. A large periampullary tumor with long, indolent history, absence of jaundice and imaging features of an expansive growth pattern, pushing rather than invading major vascular structures is likely to be benign (Figure A). This is well supported by PD specimen surgical pathology report of benign gastrointestinal stromal tumor of the duodenum (CD 117 positive; mitotic activity < 2 / 50 per high power field). Therefore PC is also ruled out
Of the remaining two options with high SAAG ascites, a well opacified portal and splenic vein (Figure B, image 2) on abdominal CECT excluded portal vein thrombosis (option 2) as well. Other notable findings of interest in this image include post PD pancreato-jejunal anastomosis, biliary-enteric anastomosis and an atrophic pancreas. whipple surgery
In our patient, initial plain images of abdominal CT scan show ascites with the liver having extremely low attenuation when compared to the spleen (Figure B, Image 1) highly suggestive of NAFLD. This was confirmed by Hounsfield units (HU) measurement (liver with a mean of – 3.25 HU when compared to spleen 52 HU with Liver -to- spleen attenuation ratio of – 0.0625, Figure C). In addition she had loss of weight, low serum albumin and cholesterol – regarded as characteristic of post PD NASH.2 In contradistinction conventional NASH presents with obesity and hyperlipidemia.2 The final diagnosis therefore is post PD NASH (option 4).
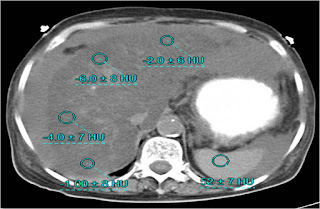
Figure C. Liver & spleen attenuation values on unenhanced abdominal computed tomography image
Following PD, NAFLD is recognized in up to 37% patients of which 10 % may progress to NASH.3 Low remnant pancreatic volume and resulting pancreatic exocrine insufficiency are some of the proposed risk factors. Management is primarily supportive and the mainstay of therapy includes high protein calorie diet, pancreatic enzyme replacement and diuretics.
References
- Van der Gaag NA, Verhaar AC, Haverkort EB, Busch OR, van Gulik TM, Gouma DJ. Chylous ascites after pancreaticoduodenectomy: introduction of a grading system. J Am Coll Surg;207:751-7
- Tanaka N, Horiuchi A, Yokoyama T, Kaneko G, Horigome N, Yamura T et al. Clinical characteristics of de novo nonalcoholic fatty liver disease following pancreaticoduodenectomy. J Gastroenterol 2011;46:758-68
- Kato H, Isaji S, Azumi Y, Kishiwada M, Hamada T, Mizuno S et al. Development of nonalcoholic fatty liver disease(NAFLD) and nonalcoholic steatohepatitis (NASH) after pancreaticoduodenectomy: proposal of a postoperative NAFLD scoring system. J Hepatobiliary Pancreat Sci 2010;17:296-304
Authors:
Dr Nitin Vashistha, MS, FIAGES, FACS
Dr Dinesh Singhal, MS, FACS, DNB (Surg Gastro)
Department of Surgical Gastroenterology,
Max Super Speciality Hospital, Saket, New Delhi, India
E mail: gi.cancer.india@gmail.com

