Insulinoma is a rare neuroendocrine tumor arising from insulin producing β-cells of the pancreas. Insulinoma patients present with history of abnormally low blood sugar levels associated with hypoglycemic symptoms such as visual disturbances, confusion, weakness, abnormal behaviour, sweating or palpitations. In severe cases patient may develop seizures, loss of consciousness or may go into coma. The triad of any of these symptoms on fasting together with hypoglycaemia (blood sugar < 40 mg%) and relief of symptoms on intake of sugars is known as Whipple’s triad, which is suggestive of insulinoma. Diagnosis of insulinoma is confirmed by evocative testing, when fasting blood sugar is ≤ 40 mg% is associated with hyperinsulinemia (> 23µU/ml) and raised C-peptide levels (> 4.4 ng/ml).1
Once a diagnosis of insulinoma has been made the next most important is to localize the tumor within the pancreas for surgical planning. Owing to hyper-vascular nature, on contrast enhanced CT scan (Figure 1), insulinoma typically appear as hyperattenuating nodule with clear margins and avid enhancement in comparison to normal pancreatic parenchyma on post-contrast arterial or pancreatic phase images 2.
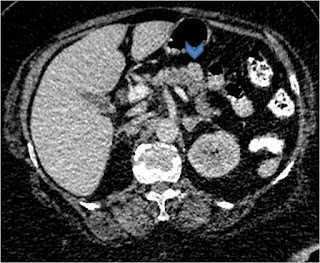
Figure 1. Abdominal contrast enhanced computed tomography scan (Arrow head pointing towards insulinoma)
While in the past preoperative localization of insulinoma was difficult but now with modern high-resolution, multi-phase contrast enhanced thin slice cross sectional-imaging (CT scan, MRI) and endoscopic ultrasonography high preoperative localization rates are feasible. In rare instances when preoperative localization of tumor is unsuccessful then intraoperative ultrasound is a useful adjunct for localization of the tumor.
Insulinoma are mostly sporadic (94%), benign (87%) and solitary (90%) and are mostly smaller than 20 mm in diameter (84%).3 Surgery is curative for patients with insulinoma and resection of localized insulinoma results in biochemical cure in 98% patients with 6% chances of recurrence at 10 years.4 The two surgical options for benign insulinoma include enucleation or segmental resection. Both the surgical procedures are safe and for an individual patient choice of the surgical procedure is based on the size & location of the tumor.
Enucleation (Figure 2) is commonly performed procedure because of its advantage of preserving pancreatic parenchyma.
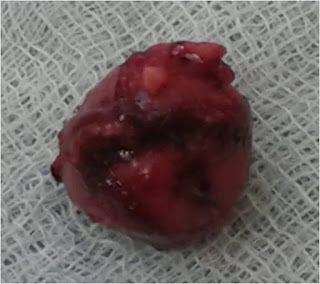
Figure 2. Enucleated insulinoma (tumor from Figure 1)
Complete removal of the insulinoma is important for preventing recurrence.5 Enucleation is safe for small lesions which are > 2 mm away from the main pancreatic duct.6 Enucleation is associated with less blood loss, shorter hospital stay and lower rates of exocrine & endocrine insufficiency in comparison to segmental resection. Although rate of postoperative pancreatic fistula (POPF) is reported to be higher after enucleation but increased POPF rates are not associated with higher mortality or morbidity.7
Segmental resection of pancreas i.e. pancreaticoduodenectomy, central pancreatectomy or distal pancreatectomy (Figure 3) is indicated for lesions in close proximity to the main pancreatic duct, deeply situated tumors in pancreas and when there is suspicion of malignancy. In various reports rate of segmental resection of pancreas for insulinoma is reported to be indicated in around 50% of the patients.8
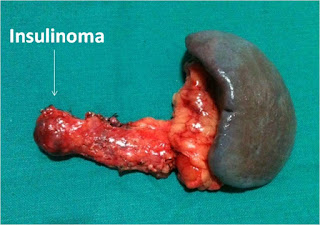
Figure 3. Distal pancreatectomy specimen
In summary surgery is curative for benign insulinoma and outcomes of both enucleation and segmental resection are comparable. Wherever feasible enucleation may be preferred over segmental resection. Enucleation is associated with improved exocrine and endocrine function but with a higher rate of POPF without increased mortality or overall morbidity rates.
References
- Vashistha N, Aggarwal B, Singhal D. Young adult with multivisceral lesions and hypoglycaemia. Gastroenterology. 2016;151(1): 43-44
- Zhu L, Xue H, Sun H et al. Insulinoma Detection With MDCT: Is There a Role for Whole-Pancreas Perfusion? Am J Roentgenol. 2017;208: 306-314
- Mehrabi A, Fischer L, Hafezi M et al. A Systematic Review of Localization, Surgical Treatment Options, and Outcome of Insulinoma. Pancreas.2014;43(5):675–686, JULY
- Howe JR, Merchant NB, Conrad C et al. The North American Neuroendocrine Tumor Society Consensus Paper on the Surgical Management of Pancreatic Neuroendocrine Tumors. Pancreas. 2020; 49(1):1-33
- Mathur A, Gorden P, Libutti SK. Insulinoma. Surg Clin North Am. 2009; 89(5): 1105–1121
- Brient C, Regenet N, Sulpice L et al. Risk factors for postoperative pancreatic fistulisation subsequent to enucleation. J Gastrointest Surg. 2012;16(10):1883-7
- Huttner FJ, Koessler EJ, Hackert T et al. Meta-analysis of surgical outcome after enucleation versus standard resection for pancreatic neoplasms. Br J Surg. 2015;102 (9), 1026-36
- Crippa S, Zerbi A, Boninsegna L et al. Surgical Management of Insulinomas Short- and Long-term Outcomes After Enucleations and Pancreatic Resections. Arch Surg. 2012;147(3):261-266
Authors:
Dr Nitin Vashistha, MS, FIAGES, FACS
Dr Dinesh Singhal, MS, FACS, DNB (Surg Gastro)
Department of Surgical Gastroenterology,
Max Super Speciality Hospital, Saket, New Delhi, India
E mail: gi.cancer.india@gmail.com

